Unexpected Skin Darkening: When Medication Causes Hyperpigmentation
Introduction
Imagine waking up one day to find patches of your skin turning an unnerving shade of black and blue. For one woman, this startling change appeared just weeks after starting a new medication. Her experience is a striking reminder that the drugs we take can sometimes trigger unexpected reactions, including alterations in skin pigmentation. This article explores the phenomenon of drug-induced hyperpigmentation, its common causes, and how it can be managed.
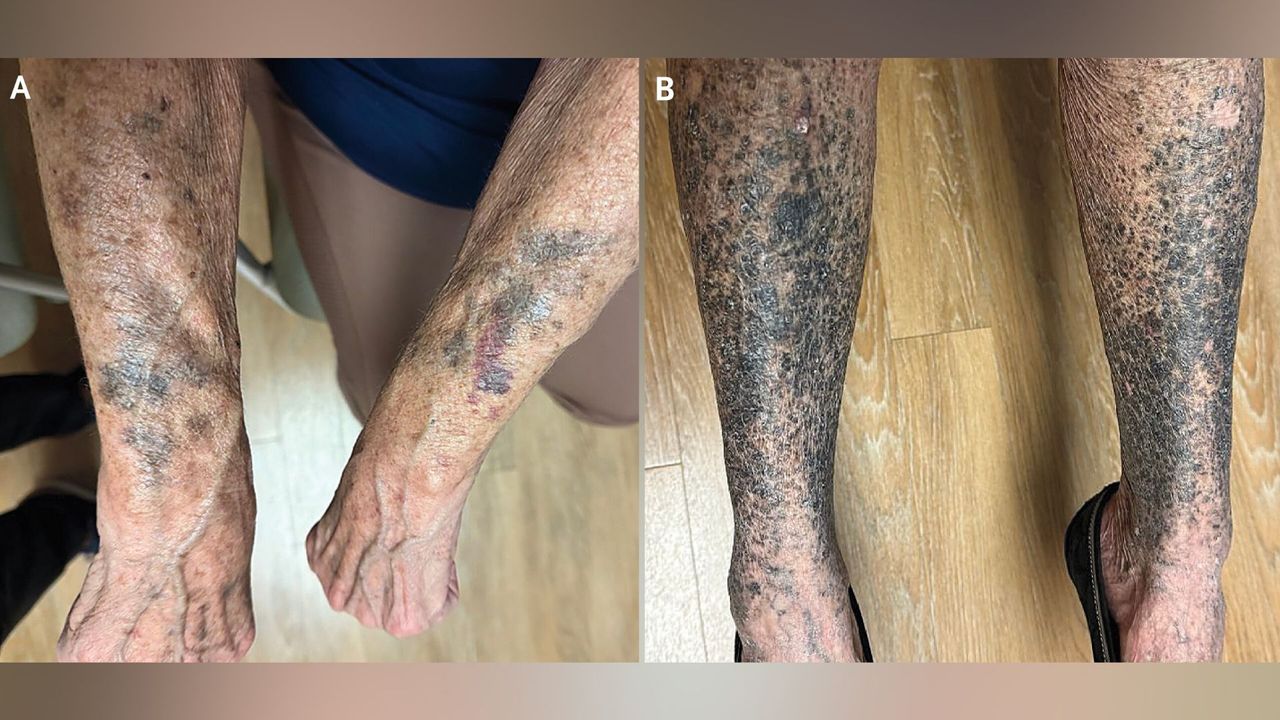
The Case: A Sudden Shift in Skin Color
A woman in her 40s sought medical help after noticing dark, bluish-black patches spreading across her arms and torso. The discoloration began gradually, about three weeks after she began a new prescription for a chronic condition. Labs ruled out autoimmune disorders and blood clotting issues, leading her doctors to a surprising conclusion: the new medication was to blame. Upon discontinuing the drug and starting an alternative therapy, her skin gradually returned to its normal tone over several months.
Her case illustrates a classic diagnostic dilemma—when a medication’s side effect mimics other skin conditions. Drug-induced hyperpigmentation is often reversible if caught early, but it requires both patient and physician awareness.
Understanding Drug-Induced Hyperpigmentation
Hyperpigmentation is the darkening of an area of skin caused by increased melanin production or deposition of the drug or its metabolites. Medications can trigger this response through several mechanisms:
- Melanocyte stimulation: Some drugs directly stimulate melanin-producing cells.
- Drug-metal complexes: Certain medications bind to metals in the skin, creating dark deposits.
- Photosensitivity: Some drugs make skin more sensitive to sunlight, leading to pigmentation in exposed areas.
- Post-inflammatory changes: Drug rashes or inflammation can leave behind dark marks.
The resulting discoloration can be slate-gray, brown, blue-black, or purplish, depending on the drug and the depth of pigment in the skin layers.
Common Culprits: Medications That May Cause Discoloration
While hundreds of drugs can affect skin color, a few are particularly notorious:
- Minocycline: This antibiotic used for acne and infections can cause blue-black pigmentation on the shins, nails, and even inside the mouth.
- Antimalarials (e.g., hydroxychloroquine, chloroquine): Used for lupus and rheumatoid arthritis, these can produce slate-gray hyperpigmentation on the face and arms.
- Chemotherapy agents (e.g., bleomycin, cyclophosphamide): Can cause diffuse darkening or linear streaks along veins.
- Hormonal therapies (e.g., oral contraceptives, hormone replacement therapy): May trigger melasma-like patches on the face.
- Psychotropic drugs (e.g., chlorpromazine, imipramine): Can lead to bluish discoloration in sun-exposed areas after long-term use.
- Amiodarone: A heart medication that can cause a distinctive blue-gray pigmentation on sun-exposed skin.
Even over-the-counter products like non-steroidal anti-inflammatory drugs (NSAIDs) have been linked, though less commonly.
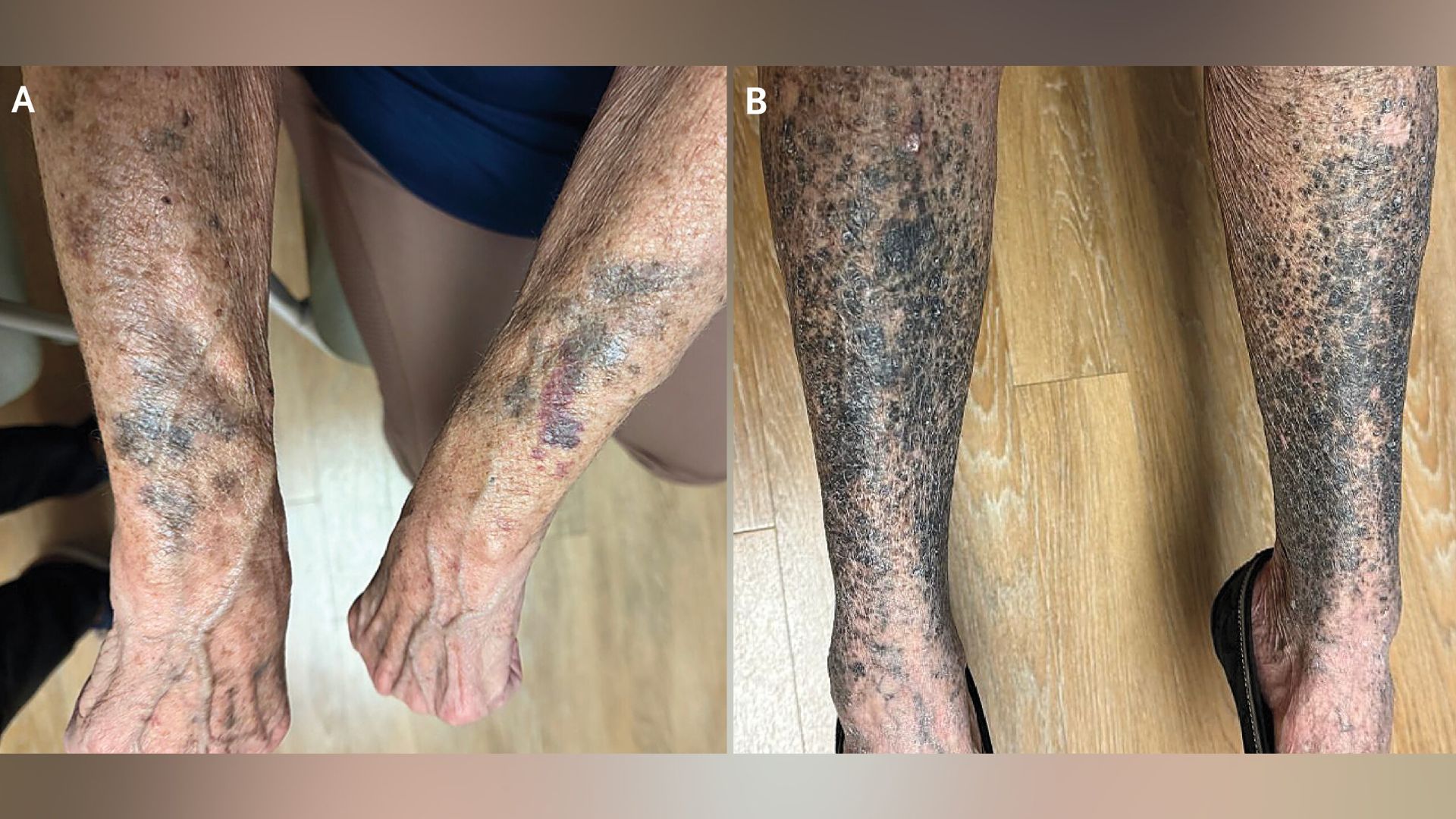
Diagnosis and Management: What to Do If You Notice Changes
If you develop new areas of skin darkening, especially after starting a new medication, consider these steps:
- Document the onset: Note when the pigmentation appeared and how quickly it spread.
- Review your medications: Make a list of all drugs, supplements, and herbal remedies you are taking.
- Consult a healthcare professional: A dermatologist or primary care physician can evaluate the pattern and consider a skin biopsy if needed.
- Assess sun exposure: Since many drug-induced pigmentations are photosensitive, wearing sunscreen and protective clothing is crucial.
Once the culprit drug is identified, the first step is usually to stop or switch the medication under medical supervision. In most cases, the discoloration fades over weeks to months, though some pigment may persist indefinitely. Topical treatments like retinoids, hydroquinone, or laser therapy may help speed resolution, but they are secondary to eliminating the cause.
When to Seek Help: Recognizing Red Flags
While medication-induced hyperpigmentation is usually benign, certain signs warrant prompt evaluation:
- Rapidly spreading patches
- Blisters, itching, or pain
- Involvement of mucous membranes (mouth, eyes, genitals)
- Accompanied by other symptoms like fever, joint pain, or fatigue—which could indicate a more serious systemic reaction
If you experience any of these, seek medical attention immediately to rule out conditions like Stevens-Johnson syndrome or drug-induced lupus.
Conclusion
The woman who turned “black and blue” from her medication is a powerful example of how drugs can affect the skin in unexpected ways. Drug-induced hyperpigmentation is a well-recognized but often overlooked side effect. By being vigilant about changes in your skin and communicating openly with your healthcare team, you can catch these reactions early and minimize their impact. Remember, not all skin darkening is sun-related—it could be a sign that a medication is leaving its mark in more ways than one.
Related Articles
- Revolutionary Injectable Hydrogel: A Step-by-Step Guide to Intravenous Tissue Repair
- How to Channel Your Inner J. Craig Venter: A Step-by-Step Guide to Revolutionizing Biotechnology
- The Silver Screen's Hidden Influence: How Media Portrayals Shape Health Behaviors
- Gene-Silencing DNA Molecules Slash LDL Cholesterol by Nearly 50% in Statin-Free Breakthrough
- How to Use AI-Powered Recommendation Algorithms to Discover Drugs for 'Undruggable' Diseases
- 7 Critical Facts About PFAS in Infant Formula You Must Know
- Ozempic and Wegovy: Untapped Mental Health Benefits Revealed in Decade-Long Study
- How to Access DFMO Treatment for Bachmann-Bupp Syndrome: A Step-by-Step Guide